[CLICK DOWNLOAD TO SEE COMPLETE ALGORITHM ILLUSTRATION]
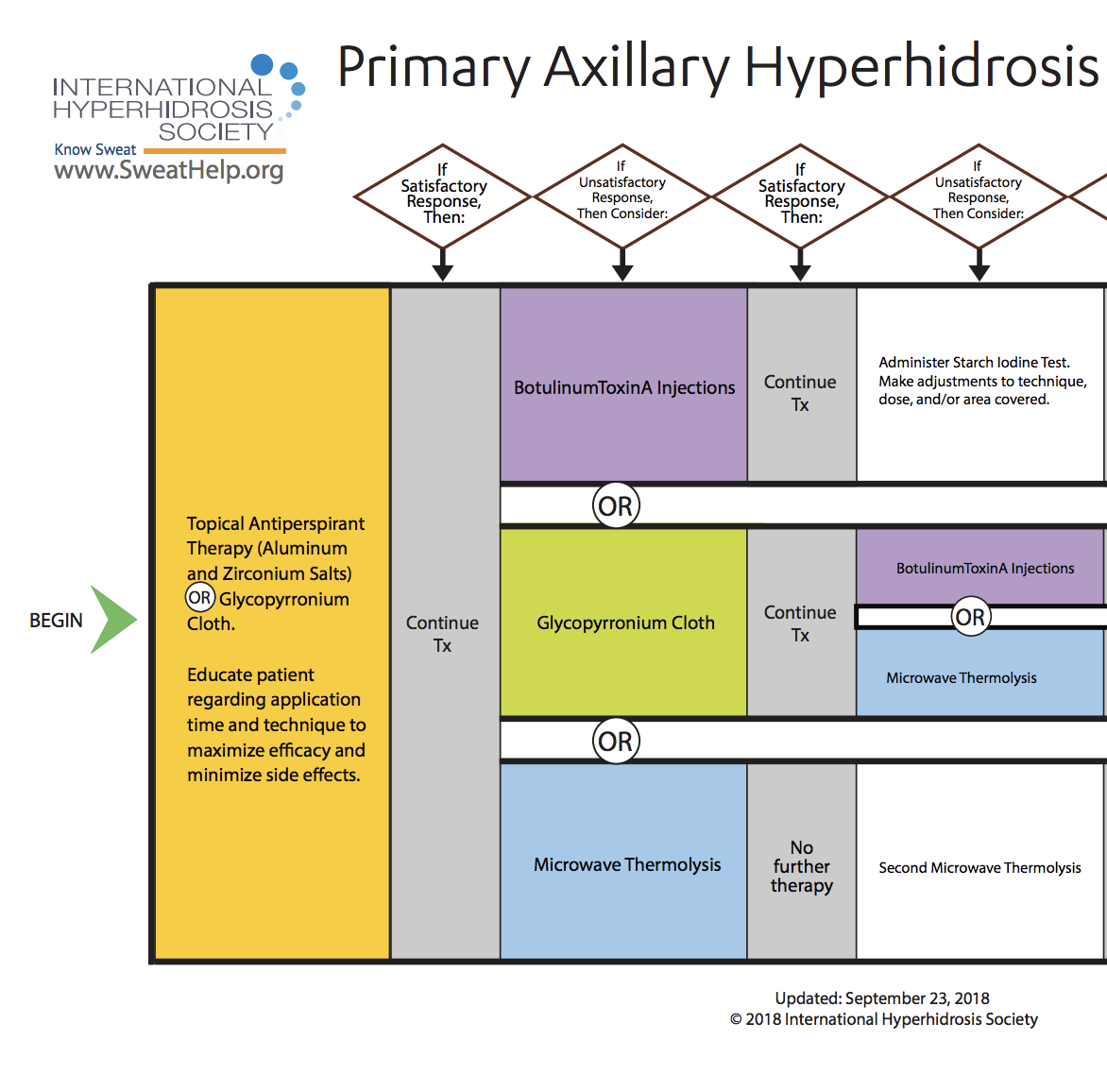
When approaching treatment to primary focal axillary hyperhidrosis, the general recommendation is to try more conservative therapy before resorting to invasive treatment. While each of the anatomic areas prone to excessive sweating is more or less susceptible to the various approaches available, [9] treatment guidelines for primary focal axillary hyperhidrosis are as follows:
For many patients, treatment will begin with topical antiperspirants starting with over-the-counter "clinical strength" products (active ingredient often zirconium salts) and then prescription products (active ingredient often aluminum chloride hexahydrate). Indeed, topical aluminum chloride hexahydrate formulations have long been, and continue to be, the first line of treatment for axillary hyperhidrosis. [9,58] Typically, aluminum chloride hexahydrate 20% solution is the most commonly prescribed agent. These topical antiperspirants can be very effective, but are limited by irritation that is caused by the formation of hydrochloric acid in a chemical reaction between the aluminum chloride and sweat present on the skin surface. Application on a very dry, nonoccluded skin surface can reduce this irritation substantially. [154,13]
Generally, it's recommended that prescription antiperspirants containing aluminum chloride be applied before sleep (when sweating is at its most minimal) and washed off 6 to 8 hours later. Skin should be dry and completely sweat-free before product application [157] -- a cool blow drier or towel may be used if necessary. Washing the skin before application is not necessary and may actually lead to greater irritation. If skin irritation occurs, topical hydrocortisone cream treatment is often recommended. In the absence of skin irritation, the antiperspirant should be applied every night for 1 week until sweating is reduced. Once the antiperspirant has taken effect, the period between treatment re-application may be extended to once per week, or less frequently, as long as desired results are maintained. [155]
While antiperspirants are usually recommended as first line treatment for primary axillary hyperhidrosis, there is a possible exception if the patient's excessive sweating symptoms occur during, or are exacerbated by, known anxiety-provoking situations such as presentations at work, dramatic performances, etc. In these cases, the patient may be treated prior to such events with an anticholinergic or a short course benzodiazepine. [9,19] More information regarding anticholinergic and other oral treatments may be found below.
If a patient does not adequately respond to topical antiperspirant therapy, or if the side effects of such therapy are intolerable, onabotulinumtoxinA injections are one of the next lines of treatment. The U.S. Food & Drug Administration (FDA) has approved onabotulinumtoxinA for the treatment of severe primary axillary hyperhidrosis in patients unable to obtain relief with antiperspirants (July 19, 2004). OnabotulinumtoxinA injections offer a minimally invasive treatment option and should be repeated as necessary to control symptoms. [99] The average duration of improvement is six to eight months for the axillae. [154,13] If the desired results are not achieved initially, practitioners are advised to make adjustments to technique, dose, and/or the area covered and repeat the treatment. Although some patients relapse shortly after their course of treatment, most studies report that a second set of injections will often provide effective symptom abatement. [156] For some patients and for various reasons, frequent re-injections of onabotulinumtoxinA can be impractical and other options can be considered, instead.
Cleared by the FDA in February 2011, miraDry is an electromagnetic energy/microwave technology device that, in a noninvasive manner, results in thermolysis of the sweat glands. Results have been shown to be lasting and stable through the last follow-up visit studied (12 months) [158, 6] Patients may require as few as one or as many as three processes to achieve desired results. [159, 1] See our informative webinar about miraDry.
Qbrexza (glycopyrronium) cloths are a more recent addition to the potential arsenal and received FDA approval in June 2018 for the treatment of primary axillary hyperhidrosis in patients aged 9 years and older. Qbrexza is an anticholinergic drug available as a 2.4% solution on a single-use cloth towelette, packaged in a pouch for topical administration. Qbrexza was shown in clinical trials to improve sweating symptoms as soon as 1 week after starting the regimen. Studies also found that patients using Qbrexza wipes once daily for four weeks improved their “sweating severity” by nearly 25% to 30% (compared to 4% to 5% with placebo) and that measured sweat volume was reduced by 50% or more (in most patients.) The wipes were "well-tolerated" and any reported side effects were primarily mild to moderate. The most common side effects were: dry mouth (in 16.9-24.2% of patients); erythema/area redness (in 17% of patients); and burning/stinging (in 14.1% of patients). One may review the following four research studies presented at an American Academy of Dermatology meeting to learn more about the Qbrexza safety and efficacy profile:
- Open-label study evaluating long-term safety of topical glycopyrronium tosylate (GT) in patients with primary axillary hyperhidrosis (ARIDO)
- Glycopyrronium tosylate for the treatment of primary axillary hyperhidrosis: pediatric subgroup analyses from the ATMOS-1 and ATMOS-2 phase 3 randomized controlled trials
- Topical glycopyrronium tosylate (DRM04) for the treatment of primary axillary hyperhidrosis: pooled results from the ATMOS-1 and ATMOS-2 phase 3 randomized controlled trials
- Glycopyrronium tosylate for the treatment of primary axillary hyperhidrosis: prior treatment analyses from the ATMOS-1 and ATMOS-2 phase 3 randomized controlled trials
In April 2023, the U.S. FDA cleared for use the Brella™ SweatControl Patch™ for the treatment of primary axillary hyperhidrosis. Brella™ is cleared to be applied by a healthcare provider for approximately 3 minutes and works via targeted alkali thermolysis (TAT). TAT technology is based on the principle that heat is generated when sodium meets water. The result is that when the Brella patch is applied to the underarm, there’s an interaction between the water in sweat and the sodium in the patch to generate a targeted amount of heat, causing microthermal injury to the sweat glands that inactivates those glands for a period of time. Results have been reported to last 2 to 4 months. The FDA’s clearance of Brella is based on data from SAHARA (NCT04599907), a randomized, double-blind, sham-controlled, multicenter pivotal study that included 110 adult patients with primary axillary hyperhidrosis. Brella was well tolerated among patients with no reported serious or severe adverse events. Data from the SAHARA study was presented in a late-breaking oral presentation at the 2023 American Academy of Dermatology Annual Meeting and showed that 64% of patients treated with the patch achieved Hyperhidrosis Disease Severity Scale improvement compared with 44% with placebo. Measured sweat production decreased by more than 50% for most (60%) of treated patients.
Oral systemic medications including anticholinergics (glycopyrrolate, oxybutynin, and propantheline), propranolol, clonidine, and diltiazem may be used to treat primary axillary hyperhidrosis, but require patient education regarding potential side effects (such as dry mouth, blurred vision, urinary retention, tachycardia and constipation). These side effects may limit the use of anticholinergics in many patients [154, 13, 155] but sometimes can be managed by adjusting the individual's dose. Before treatment with oral systemic medications for hyperhidrosis, extra consideration should be given regarding pediatric patients, people who participate in sports, people who work outdoors and any other patients who may potentially cause themselves injury by becoming overheated. Of interest to practitioners with pediatric patients, the FDA has approved (July 2010) a liquid form of the anticholinergic glycopyrrolate (brand name, Cuvposa) to reduce drooling in pediatric cerebral palsy patients – off-label use of this medication may provide flexibility when dosing for pediatric patients. Watch our expert-led webinar about oral medications to treat hyperhidrosis.
Additional treatment options for primary axillary hyperhidrosis include local surgical procedures: excision, curettage, liposuction, and laser. Combinations of curettage and central excision, or of curettage and liposuction may be used, as well as combinations of liposuction and laser treatments. Complete excision of underarm tissue containing sweat glands is no longer recommended because scarring can cause range of motion limitations. [155, 156] If sweat reduction has not been sufficient after local surgical treatment, a procedure may be repeated or onabotulinumtoxinA or antiperspirants may be used to control sweating from remaining sweat glands. [7,99]
Finally, for carefully selected patients, endoscopic thoracic sympathectomy (ETS) may be an option if all other treatment options have been exhausted (including rounds of treatment regimen adjustments, retreatment, and combination therapies). It should be recognized, however, that sympathectomy has been shown to be effective for palmar sweating, but is less effective for axillary symptoms. If ETS is to be pursued, patients must be educated to fully understand the possibility of limited efficacy and the risk of complications including, but not limited to, compensatory sweating. [9] See our informative webinar about miraDry here.